Vein Disease
Vein Disease
Do you suffer from varicose veins? Do you experience aching leg pain and discomfort? Do you have leg swelling?
The good news is you are not alone. Over 50-80 million Americans suffer from an underlying condition called chronic venous insufficiency with symptoms such as varicose veins, leg pain, swelling, and discomfort.
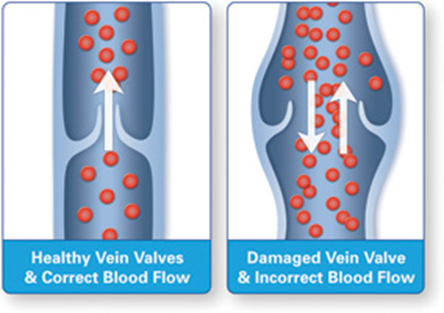
What is chronic venous insufficiency?
In healthy functioning veins, small valves inside of the vein allow blood to flow in one direction back to the heart. Chronic venous insufficiency is a medical condition where these valves become damaged or weakened and do not close properly which allows blood to flow downward back into the vein. This is also called venous reflux, which results in blood pooling in the legs and ankles and the veins to bulge. Common symptoms of chronic venous insufficiency may include varicose veins, pain, swelling, itching, and flaking skin, skin discoloration, heavy legs, restless legs, and skin ulcerations.
Risk factors associated with chronic venous insufficiency include family history, pregnancy, obesity, and/or a lifestyle or profession that includes prolonged periods of standing or sitting.
Symptoms
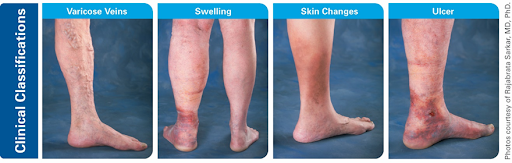
Common symptoms of vein disease can range from small cosmetic issues to more severe leg pain or physically limiting conditions including ulcers or immobility. Often times cosmetic issues seen on the skin’s surface are just indicators of a deeper, underlying condition such as chronic venous insufficiency.
Common symptoms include:
Spider veins (telangiectasia)
Spider veins are tiny, thin, red/blue/green colored veins close to the skins surface. These veins become non-functional, dead-end veins. Spider veins themselves are primarily unsightly and do not usually cause discomfort. Many vein disease sufferers have a combination of spider veins and varicose veins.
Varicose veins (bulging, ropy veins)
Varicose veins are enlarged veins that appear bulging and ropy. They are often deeper in the leg and may not always be visible on the skin. Family history is a common risk factor in those suffering with varicose veins. Pregnancy, obesity, and occupations that require prolonged periods of standing or sitting are other common risk factors.
Leg pain, aching, or heaviness
People with vein disease and varicose veins often suffer with a dull, heavy ache in their legs. Some describe it as tiredness or heaviness in the legs without any visual signs of vein disease. The pain or heaviness in the legs may worsen at night, or after extended periods of standing or sitting.
Itching, red rash, or flaking skin (dermatitis)
Itching, red rash, or flaking skin on the legs can be a sign of underlying vein disease. People may also experience a burning sensation, throbbing, and skin that may feel slightly numb or warm to the touch.
Leg swelling (lymphedema)
A common sign of vein disease is edema, or swelling, often experienced in the lower legs, calves, ankles, and feet. The swelling may be a sign that the veins are not working properly causing fluid accumulation. In addition to leg or ankle swelling, edema can lead to changes in skin color and/or severe pain and discomfort in the lower limbs.
Leg cramping
Leg cramping is an extremely common symptom of vein disease. The leg cramping may be a sign of the veins not working properly and the fluid accumulation can lead to the leg muscles contracting or cramping. The leg cramps may worsen at night, or after lengthy periods of standing or sitting.
Ankle sores (leg ulcers)
The most severe stage of vein disease is leg wounds or leg ulcers. Leg ulcers in most patients result from underlying vein disease. Poor circulation and pooling of fluid in the lower limbs caused by untreated vein disease may result in ulcers forming.
Restless legs syndrome (RLS)
People with vein disease often describe experiencing leg restlessness, or the constant urge to move their legs. These symptoms often occur or worsen at night.
Skin discoloration (hyperpigmentation, lipodermatosclerosis)
Skin discoloration may be experienced in advanced stages of vein disease. The skin changes result from the poor circulation and pooling of fluids that cause increased pressure inside the vein walls.
Blood clots (thrombosis, deep vein thrombosis (DVT), thrombophlebitis)
Leg veins may become inflamed or painful, a condition called superficial phlebitis, which can be associated with vein thrombosis, or blood clots. Deep vein thrombosis, or DVT, affects the larger veins deep in the lower leg and thigh. DVT, though rare, can be life-threatening if the blood clot breaks off and travels to the lungs.
Vein disease is a progressive, medical condition that may worsen to more serious concerns if left untreated. It is best to speak with a vein specialist if you are experiencing any of the symptoms listed above and identify the appropriate treatment plan for you.
A vein specialist may recommend one or more of the following treatments:
Ultrasound Exam
A complete ultrasound exam is an important first step in successfully treating venous disease. A thorough ultrasound exam will be completed during the initial exam to identify underlying chronic venous insufficiency, which may be causing other symptoms. Ultrasound is often used during the treatment and post-procedure to confirm results and to rule out any complications. Routine ultrasound exams are part of follow-up visits at CVD to track progress and ensure a successful treatment.
Sclerotherapy
Sclerotherapy is often the treatment for spider veins and small varicose veins closer to the skin surface. With sclerotherapy, a solution is injected into the varicose or spider veins, which causes them to seal off and close over time eventually being absorbed into the body. Blood is rerouted to healthy veins in the leg. A vein light or ultrasound guidance may be used to assist in the delivery of the solution. Sclerotherapy is usually considered a cosmetic procedure and used in conjunction with other therapies to treat the underlying venous disease
Radiofrequency and Endovenous Laser Vein Ablation
Radiofrequency (RF) and Endovenous laser vein ablation are used to treat chronic venous insufficiency, the underlying cause of varicose veins and other symptoms. A thin catheter is inserted into the diseased vein and radiofrequency energy (heat) is applied to the inside of the vein causing the vein wall to collapse and form a fibrotic seal. Over time the body absorbs the vein tissue. Blood is rerouted to healthy leg veins. The Center for Venous Disease has performed thousands of these procedures with a 98% success rate making us the most experienced vein center in the Southwest United States. CVD is a VNUS™ Certified Training Site. CVD vein specialists prefer radiofrequency ablation to laser ablation when treating vein disease due to the significantly less pain, bruising, tenderness, and adverse events following treatment. Most patients experience relief from the pain associated with venous disease following radiofrequency ablation. The recovery period is minimal with most people returning to normal activities within 1-2 days. An additional procedure such as sclerotherapy may be done following the ablation treatment to address any residual spider veins or cosmetic concerns.
Deep Vein Thrombosis (DVT) Screening
Deep vein thrombosis, or DVT, is a blood clot that affects the larger veins deep in the lower leg and thigh. DVT, though rare, can be life-threatening if the blood clot breaks off and travels to the lungs. During the initial exam, an ultrasound is used to rule out DVT. Also following any vein procedure, a follow-up appointment including a DVT screening using ultrasound will be required. A physician may recommend an annual DVT screening as part of your wellness plan.
Perforator Vein Treatment
Perforator veins connect the superficial venous system to the deep venous system. If the valves in the perforator veins become damaged it can cause the superficial venous system to work poorly and cause varicose veins and other associated symptoms. As part of a commitment to Total Vein Care it is important to diagnose and treat the full disease to achieve complete symptom relief and long-term results. The Center for Venous Disease physicians use the RFSStylet™ from Medtronic. Endovenous laser is also used. Both are FDA cleared medical devices approved for energy-based treatment of refluxing or diseased perforator veins.
Wound Care
Venous ulcers, or open wounds, may occur with advanced stages of venous disease, especially when the condition is left untreated. Wound care to treat venous ulcers requires debridement of any dead tissue in the wound. This will help the ulcer heal. Another procedure to treat the underlying chronic venous insufficiency would be used in conjunction to help prevent future ulcers from developing.
Cosmetic Laser
Cosmetic laser treatment is used to treat small spider veins on the skin surface. These veins are most common on the legs though may also be seen on the face, in particular the cheeks and nose. The cosmetic laser treatment does not resolve underlying vein disease that may be causing the spider veins. It is important to address any underlying vein disease before treating cosmetic concerns.
Compression Stockings
Most insurance companies require the use of compression hose as the first step in treating vein disease to see if symptoms improve before approving any other treatments. Compression stockings are also required before and after treatment of varicose veins to help reduce the risk of blood clots post-procedure.

